A mother who lost her baby to a rare genetic disease says his life could have been saved by a test costing just £2.50.

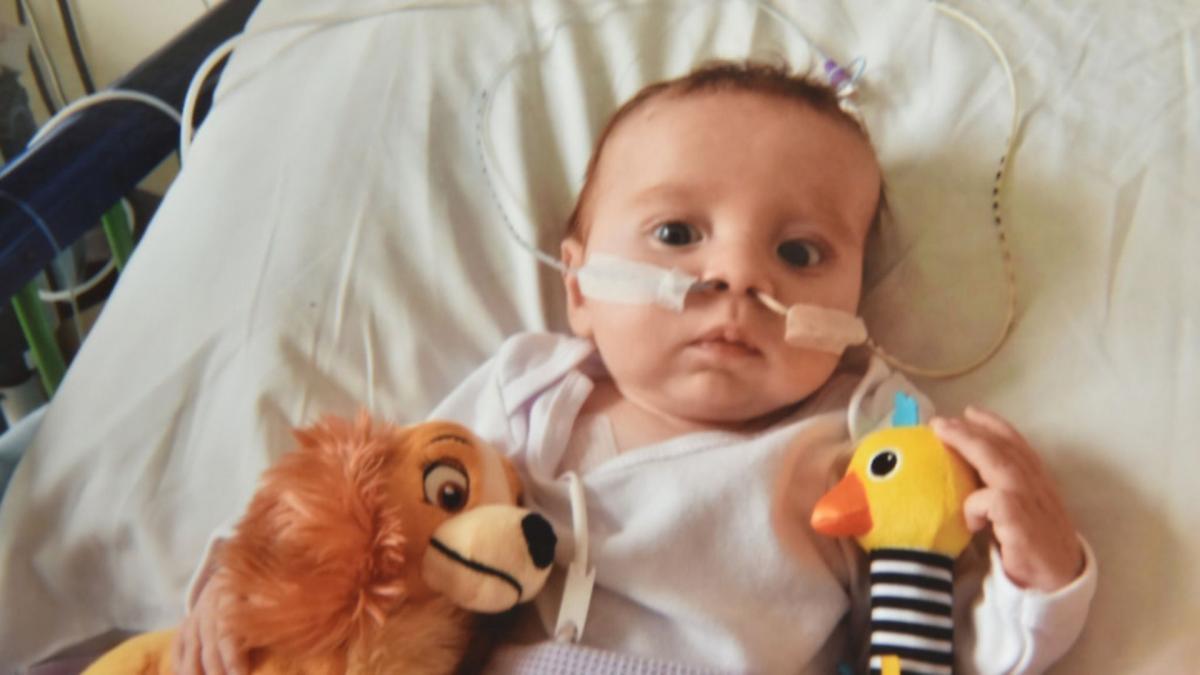
Susie Ash and her fiancé Justin Thorndyke from Forncett St Mary, near Diss, say they have gone through unimaginable grief since the death of their son, James, just before his first birthday.
And their loss has been made even more difficult with the knowledge that a simple heel-prick test to detect Severe Combined Immunodeficiency (SCID) could have saved their son's life.
Professor Bobby Gaspar, from Great Ormond Street Hospital, said screening would diagnosed James at birth and meant he could have been successfully treated for the condition.
Susie has now set up a petition to raise awareness about SCID and to push for the test to be added to newborn screening - in one week it gained 2,416 signatures.

She hopes that people in Norfolk and beyond will sign it to put pressure on the government to make a simple change and save babies' lives.
'James died in my arms on the sofa at home,' she said.
'It is the hardest thing I've ever had to do to watch my baby take his last breath.
'It was so unnecessary - that's the hard thing. Just for the sake of a £2.50 test which every parent would willingly pay for their child.'

The bereaved mother described how every day is now a nightmare and when she passes her baby's bedroom she feels lost and alone.
'SCID needs to be in the newborn screening - I don't see why there is even a question about it,' she said.
'There also needs to be raised awareness about the disease - not just with the public but doctors too.
'If James' condition had been picked up straight away I think he would still be with us today.'

She added: 'The screening committee needs to stand up to its responsibility and include SCID in newborn screening. How many more babies need to die?
'So many countries already include this screening. We are the UK - how have we fallen so behind other countries?'
James was born a healthy baby weighing in at 81bs 8oz and there were no immediate signs that anything was wrong.
But after his first set of immunisations at eight weeks old he developed a cough and had to be treated at the Norwich and Norfolk Hospital for pneumonia.

After returning home he became steadily worse - he stopped feeding and smiling and became lethargic. He was readmitted to hospital where he started to have seizures, became lifeless and stopped crying.
He was transferred to Addenbrooke's Hospital where he was diagnosed with SCID, and then moved again to Great Ormond Street Hospital.
James was put on a ventilator for three weeks in quarantine and the doctors were very concerned because he was so riddled with infection.
His parents remained with him at Great Ormond Street taking it in turns to sleep next to him each night.

'It was so hard to be away from my other children - I had never been away from them for more than one night,' Miss Ash said.
'On the other hand it was what James needed. He was such a fighter, he proved the doctors wrong so many times. He so wanted to be here.'
James eventually came off the ventilator and was able to breathe all by himself.
A bone marrow transplant offered the only long-term cure but James was too sick to have the chemotherapy that went along with it.

Instead his daddy Justin donated his T-cells which were engrafted into James in the hope they would create part of his failing immune system.
James seem to be making good progress but when he came home to spend Christmas with his family he became very ill again
He was readmitted to Great Ormond Street Hospital where scans showed the transplant had not worked.
Susie and Justin were advised to take their son home, and James lost his fight to live on February 18 2017.

The petition can ben found here: www.change.org/p/uk-newborn-screening-committee-stop-the-unnecessary-deaths-of-babies-and-include-scid-in-new-born-screening-programmeBackground about SCID
Severe combined immunodeficiency (SCID) is an early childhood genetic disease which means babies are born with a defective immune system.
Infants with the disease are usually aged between three and six months and endure severe and repeated infections - without effective intervention most children will die before they are one.
Bone marrow transplantation or gene therapy can be used as a cure in these cases but has a 90pc higher survival outcome when babies are diagnosed at birth and treated before they develop any infections.
This requires the use of a biomarker called a TREC - TRECs can be detected from a routine heel-prick dried blood spot which costs just £2.50.
Newborn screening programmes using TREC are now underway in 40 states in the USA, nationally in Israel, approved for national use in The Netherlands and New Zealand and in regional or pilot programmes in Norway, Sweden, France, Spain, Germany.
Screening programme
Professor Bobby Gaspar of Great Ormond Street Hospital has been working on getting a national screening programme for SCID implemented for the past five years.
He says it is devastating for the 20 babies born a year with the condition not to have immediate access to the simple heel-prick test at birth.
Early detection takes the survival rate and capacity to live a normal life from 50pc to more than 90.
'If we don't screen, half of these would lose their lives which is what happened to Susie Ash's son,' Prof Gaspar said.
'It is not just the cost to the children but to the families too. They go through an awful lot and you can't quantify that, especially in this case.
'If we had diagnosed James at birth and put him on antibiotics and then done a bone marrow transplant the outcome could have been very different.'



Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules here